
It's 5:32pm. Your reception team has just wrapped up a full day of coordinating appointments, fielding calls, and supporting clinical staff. The phones stop being answered. And somewhere out there, a patient who finally worked up the courage to book, or a GP making a referral on behalf of a patient, hits voicemail.
They may not call back.
For specialist clinics operating with lean admin teams, this is one of the most consistent gaps in specialist clinic patient communication: the window between when patients need to reach you and when your team is actually available to answer.
This is the story of one Auckland-based specialist clinic that identified that gap, fixed it, and gave their team back hours of time in the process.
What You'll Learn
Why small, specialist clinics are disproportionately affected by after-hours and high-volume call gaps
How missed and mismanaged calls affect both patients and practice managers
What a real NZ specialist clinic changed — and the results they measured
How to assess whether your clinic has the same problem
The Hidden Cost of Missed Calls in Specialist Clinics
Specialist clinics operate differently from general practice. Your patient journey is usually longer. Booking intent is more deliberate. A patient calling your clinic, or a GP referring one, has often already made a decision. They're not browsing options. They're ready to act.
That makes every missed call more costly than it looks on paper.
When a prospective patient calls and hits voicemail, the friction is rarely just about timing. It signals to them that reaching you is going to be hard. Some will try again. Many won't.
For the Auckland vasectomy clinic at the centre of this case study, that dynamic was playing out daily. Patients calling outside business hours had no way to connect. Voicemails accumulated overnight. And by the time staff worked through them the next morning, the window to respond promptly, and professionally, had already closed.
Why Specialist Clinics Struggle More With This Than They Realise
The challenge isn't unique to this clinic. It shows up consistently across specialist practices for three interconnected reasons.
Small teams carry a disproportionate communication load. Unlike a large GP clinic with multiple receptionists, many specialist practices run on one or two administrative staff. When those people are with patients, on the phone, or managing clinical coordination, every additional call is a genuine interruption, not just an inconvenience.
Inquiry volume doesn't scale predictably. A single campaign, a new GP referral pathway, or even a seasonal uptick in bookings can push call volume beyond what a small team can absorb. There's rarely a buffer.
After-hours gaps are structural, not fixable by hiring. The issue isn't whether your team is good at their jobs. It's that there are simply hours of the day where no one is there to pick up, and patients don't stop having questions.
For this Auckland clinic, these pressures showed up as three distinct problems:
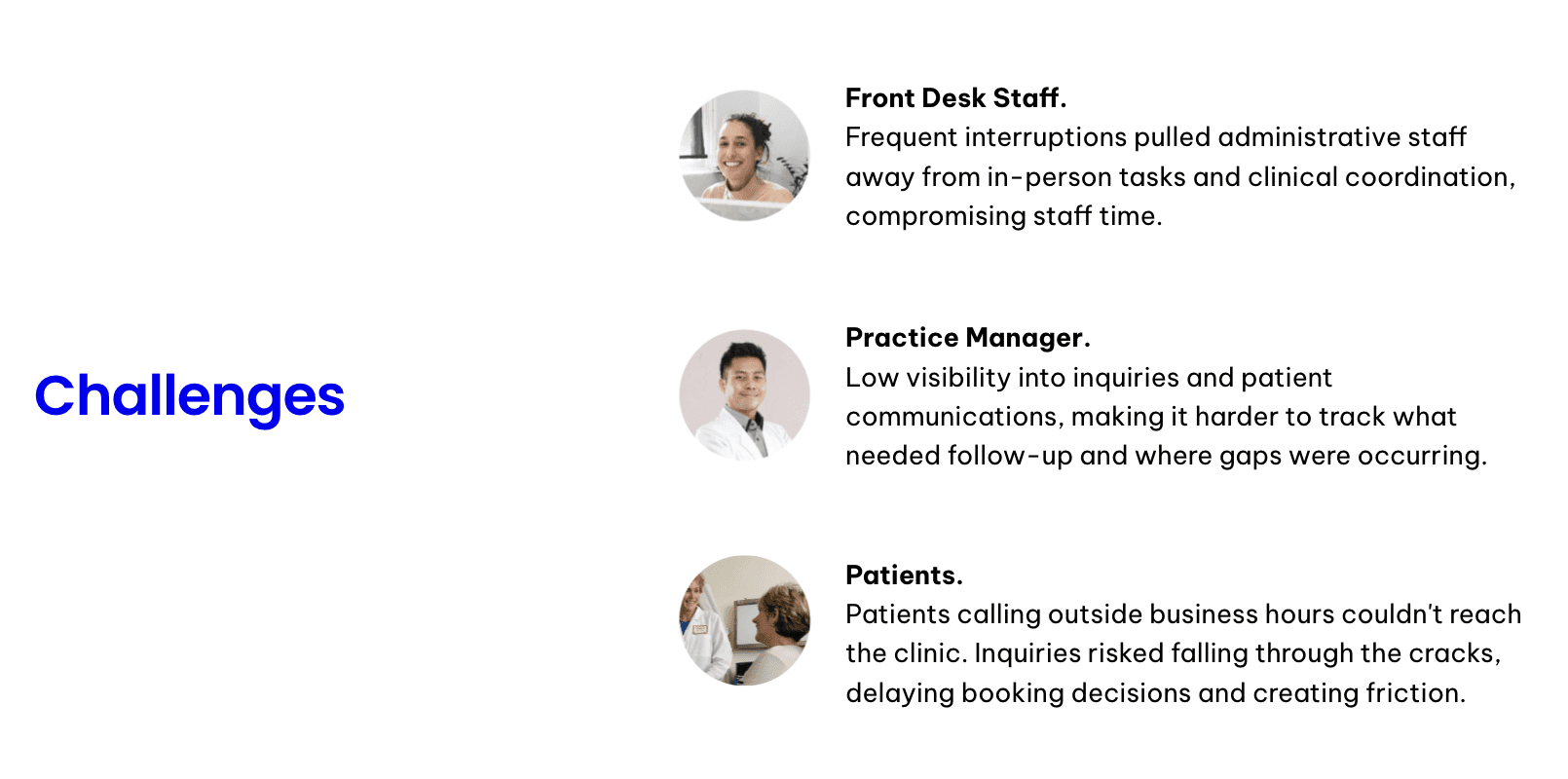
Front desk staff were being pulled away from in-person tasks and clinical coordination by frequent phone interruptions
The practice manager had low visibility into which inquiries were outstanding, which had been followed up, and where gaps were occurring
Patients calling outside business hours couldn't reach the clinic, and inquiries risked falling through the cracks before they could be actioned
What Changed: A Unified Approach to Patient Communication
The clinic's shift came from addressing all three of those problems at once, rather than treating each as a separate operational issue.
They implemented Heron — a patient communications and workflow platform built specifically for healthcare clinics — and configured it across three core functions.
24/7 Call Handling
Every inbound call is now answered, regardless of when it comes in. Patients calling outside business hours no longer hit a dead end. Nine after-hours calls were handled in the first month alone; calls that, previously, would have gone to voicemail and potentially been lost.
Auto-Transcribed Call Summaries
When a call does require staff follow-up, the team doesn't start from scratch. Every interaction is automatically transcribed and summarised, so whoever picks up the follow-up knows exactly what the patient asked, what was discussed, and what the next step is. No more playing back voicemails. No more "I'm not sure what this patient called about."
A Centralised Inquiry Dashboard
For the practice manager, visibility was the missing piece. Heron's workflow dashboard gives a complete, real-time view of every patient inquiry: where it sits, who's actioning it, and what still needs follow-up. That kind of oversight is hard to maintain when communication is scattered across a phone system, a voicemail inbox, and a notebook on the desk.

The Results After Four Months of Operation
Here's what the data showed.
Metric | Result |
|---|---|
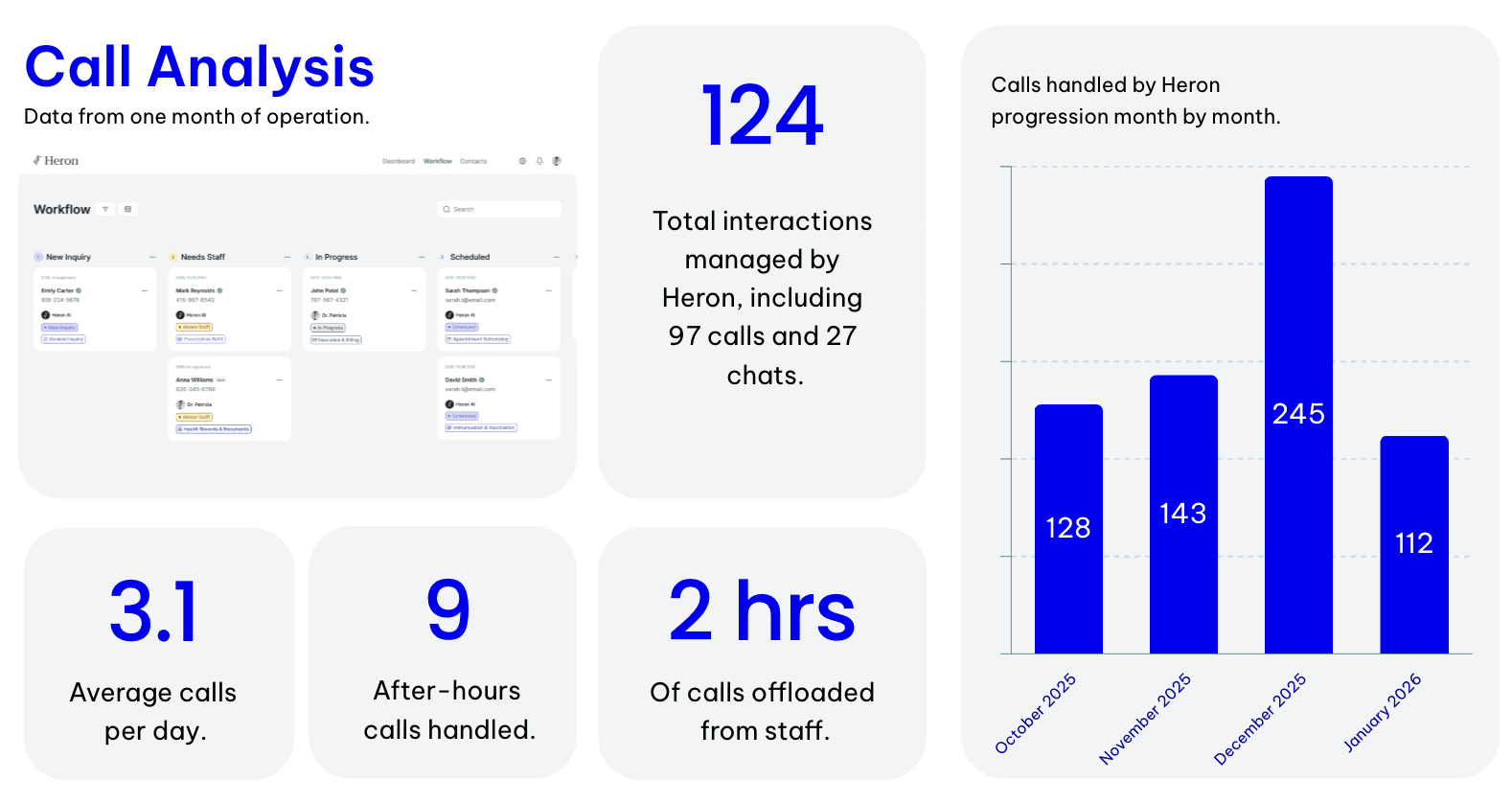
Total interactions managed | 124 in a single month (97 calls + 27 chats) |
Average calls per day | 3.1 |
After-hours calls handled | 9 |
Staff time offloaded | 2–3 hours per month |
Inquiries resolved without staff transfer | 100% |
Intent identification accuracy | 100% |
General inquiries resolved by Heron | ~60% |
That last figure matters. Roughly six in ten inquiries coming into this clinic — questions about appointments, directions, procedure information, billing — were straightforward enough to be fully resolved without a staff member needing to step in. That's not a small efficiency gain for a two-person admin team.
The practice manager put it directly:
"As a busy specialist clinic, we were losing potential patients to missed calls and after-hours voicemails that backed up overnight. Since bringing Heron on board, every call gets answered, even when our reception team is with patients or the clinic is closed. Our staff can focus on the people in front of them, and patients never feel like they've fallen through the cracks."

What This Looks Like for Your Clinic
You don't need to be a vasectomy clinic to recognise this pattern. If your practice operates with a small admin team, has patients or referring GPs who call at unpredictable hours, or struggles to give your practice manager a clear picture of outstanding follow-ups; the underlying problem is the same.
The question isn't whether your team is doing a good job. It almost certainly is. The question is whether your patient communication infrastructure is set up to support them; or whether it's quietly creating gaps that compound over time.
A few things worth checking in your own clinic:
How many calls go to voicemail in a typical week, and how quickly are they followed up?
Does your practice manager have visibility into all outstanding patient inquiries at any given moment?
When a patient calls after hours, what actually happens?
If those questions are harder to answer than they should be, the structure is the issue — not the people.
See How Heron Works for Specialist Clinics
Heron is built for exactly this kind of environment: small, high-coordination specialist practices where every patient interaction matters and every admin hour counts.
Book a Free Demo to see how the platform works for a clinic like yours.
Frequently Asked Questions
What is specialist clinic patient communication software?
Patient communication software for specialist clinics is a platform that manages inbound calls, messages, and inquiries; ensuring every patient contact is captured, categorised, and followed up. For specialist practices, this typically includes 24/7 call handling, automated summaries, and a centralised dashboard for practice managers to track outstanding inquiries.
How do specialist clinics handle after-hours patient calls?
Most specialist clinics rely on voicemail for after-hours calls, which creates a backlog for staff the following morning. Platforms like Heron handle inbound calls around the clock, ensuring patients get a response regardless of when they call and that no inquiry falls through the cracks overnight.
Why do specialist clinics miss more patient inquiries than GP clinics?
Specialist clinics typically operate with smaller admin teams and less redundancy. When staff are occupied with in-person tasks or clinical coordination, there's often no one available to cover incoming calls. This structural gap means missed calls are a common and ongoing issue, not a reflection of team performance.
How much time can better patient communication give back to clinic staff?
Based on data from one NZ specialist clinic using Heron, staff had approximately 2–3 hours of call-handling time offloaded per month, with around 60% of all inquiries resolved without requiring staff involvement. The volume of follow-up work depends on the clinic's size and call volume, but even modest reductions in repetitive call handling create meaningful capacity for front-desk teams.
What should a specialist clinic look for in a patient communication platform?
Look for a platform that covers the full communication journey: inbound call handling (including after hours), automatic logging and summarisation of inquiries, multi-channel support (calls and messages), and a dashboard that gives your practice manager real visibility into inquiry status. Integration with your existing practice management system is also important for a consistent workflow.



